By Dr. Shyam D, Board-Certified Neurosurgeon in India
Published: March 24, 2025
As a board-certified neurosurgeon with over a decade of experience in India, I’ve encountered some of the most urgent and intricate conditions of the brain—aneurysms and arteriovenous malformations (AVMs) among them. These vascular abnormalities can be silent threats or sudden emergencies, but with the right expertise, they’re manageable. In this pillar page, I’ll explain what aneurysms and AVMs are, their types, symptoms, diagnosis, and treatment options, and how my team and I help patients navigate these challenges with precision and compassion. Whether you’re a patient, caregiver, or simply curious, this guide is designed to inform and empower you.
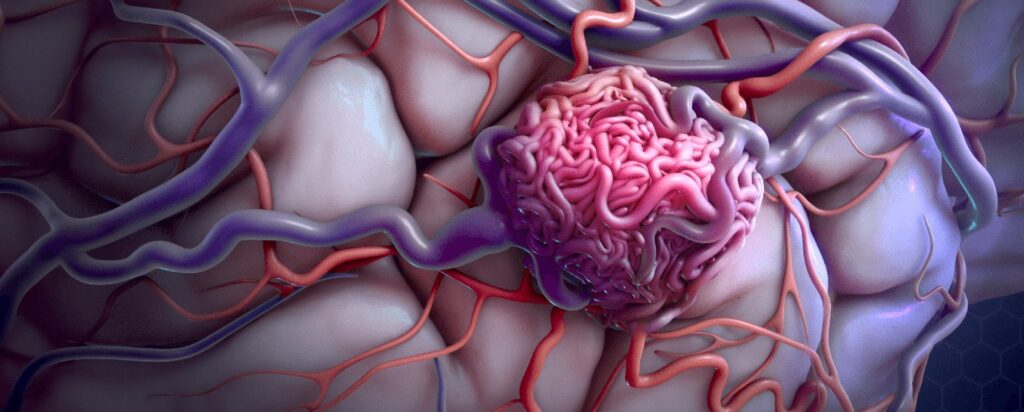
What Are Aneurysms and AVMs?
Aneurysms and AVMs are abnormalities in the blood vessels of the brain, each with distinct characteristics:
- Aneurysms: These are weakened, bulging spots in an artery wall, like a balloon ready to burst. If they rupture, they cause life-threatening bleeding (subarachnoid hemorrhage).
- Arteriovenous Malformations (AVMs): These are tangled webs of arteries and veins that bypass normal capillary systems, disrupting blood flow and risking rupture.
Over my career, I’ve treated countless cases of both—some discovered by chance, others after dramatic symptoms. My goal is to catch them early and intervene effectively.
Types of Aneurysms and AVMs
Understanding their variations helps tailor treatment. Here’s what I commonly see:
- Aneurysms
- Saccular (Berry) Aneurysms: The most common type, a small sac off an artery, often at the brain’s base (Circle of Willis).
- Fusiform Aneurysms: A diffuse widening of the entire vessel, less likely to rupture but harder to treat.
- Dissecting Aneurysms: A tear in the artery wall, rare but dangerous.
- AVMs
- Congenital AVMs: Present from birth, these vary in size from tiny tangles to large networks.
- Spetzler-Martin Grade AVMs: Classified by size, location, and drainage (Grades I-V), guiding treatment complexity.
Each type presents unique challenges. My decade of experience allows me to assess them with precision, ensuring patients get the right approach.
Symptoms of Aneurysms and AVMs
These conditions can be silent until they rupture, but warning signs often emerge:
- Aneurysms
- Unruptured: Mild headaches, vision changes (e.g., double vision), or cranial nerve issues (like drooping eyelids).
- Ruptured: Sudden, severe headache (“worst of my life”), nausea, stiff neck, seizures, or loss of consciousness.
I once treated a woman who dismissed her blurred vision—until a scan revealed a growing aneurysm pressing on her optic nerve.
- AVMs
- Unruptured: Headaches, seizures, or neurological deficits (e.g., weakness or speech trouble) due to pressure or blood flow changes.
- Ruptured: Sudden bleeding causing stroke-like symptoms—confusion, paralysis, or coma.
A young man came to me with seizures; imaging showed a small AVM. Early action prevented a catastrophic bleed.
Timing is critical—ruptures are emergencies, but even unruptured cases need attention if symptomatic.
How Are Aneurysms and AVMs Diagnosed?
Diagnosis is where my expertise as a neurosurgeon comes into play. My process is meticulous:
- Patient History & Exam: I ask about symptoms and check for neurological signs—reflexes, eye movement, strength.
- Imaging:
- CT Scans: Quick detection of bleeding from a rupture.
- MRI: Detailed views of AVM structure or unruptured aneurysms.
- Cerebral Angiography: The gold standard—injecting dye to map blood vessels, revealing size and location.
- Risk Assessment: I evaluate rupture risk based on size, location, and patient factors (e.g., smoking, hypertension).
With over ten years interpreting these scans, I can spot subtle abnormalities others might miss, ensuring accurate diagnosis.
Treatment Options for Aneurysms and AVMs
Treatment depends on the condition’s state—ruptured or not—and the patient’s health. Here’s how I approach them:
- Aneurysms
- Clipping: Surgically placing a metal clip at the aneurysm’s neck to stop blood flow. I’ve clipped aneurysms in tight spots, like the anterior communicating artery, with microsurgical precision.
- Coiling: Endovascularly inserting platinum coils to fill the aneurysm, preventing rupture. A less invasive option I often use.
- Flow Diversion: Stents redirect blood flow away from large or complex aneurysms.
- Observation: Small, asymptomatic aneurysms may be monitored with regular imaging.
- AVMs
- Surgical Resection: Removing the AVM through a craniotomy, ideal for accessible, low-grade cases.
- Embolization: Injecting glue-like material to block abnormal vessels, often a precursor to surgery or radiation.
- Stereotactic Radiosurgery: Focused radiation shrinks AVMs over time, best for deep or small ones. I’ve used Gamma Knife with great success.
- Observation: Tiny, symptom-free AVMs might be watched closely.
For a ruptured case, emergency surgery or stabilization comes first. I tailor every plan—balancing risks and benefits with patients’ needs.
How We Help Patients: Beyond the Operating Room
My work as Dr. Shyam D goes beyond fixing vessels—it’s about restoring lives. Here’s how we support patients:
- Personalized Treatment: A 40-year-old with a ruptured aneurysm got emergency coiling and rehab to return to work. A teen with a small AVM chose radiosurgery to avoid surgery’s risks. I customize care to fit each story.
- Education & Support: I explain every step—why we’re clipping, what recovery looks like—easing anxiety. My team offers counseling for emotional resilience.
- Recovery & Rehab: Post-treatment, I coordinate with therapists to address deficits—speech, movement, or cognition.
- Long-Term Care: Regular follow-ups with imaging ensure no recurrence. I’ve tracked patients for years, celebrating their milestones.
One patient—a father—survived a ruptured aneurysm thanks to swift clipping. Today, he plays with his kids again. That’s why I do this.
Risk Factors and Prevention
Aneurysms and AVMs have different origins:
- Aneurysms: Linked to hypertension, smoking, family history, or connective tissue disorders (e.g., Marfan syndrome).
- AVMs: Usually congenital, though trauma or genetics may contribute.
Prevention tips? Control blood pressure, quit smoking, and get screened if there’s family history. While AVMs can’t be prevented, early detection saves lives.
Why Choose Dr. Shyam D?
With over a decade of experience, I’ve mastered the art of treating aneurysms and AVMs—clipping delicate vessels, embolizing tangled networks—all with advanced tools like intraoperative angiography and robotics. My board certification, earned through India’s rigorous standards, and my engagement with global neurosurgery advancements (think annual conferences and research) affirm my authority. But it’s my compassionate approach—treating patients like family—that builds trust. I’ve saved lives in emergencies and preserved futures in planned cases.
Living After Aneurysms and AVMs
Outcomes vary: unruptured cases often lead to full recovery with treatment, while ruptures may leave deficits we work to overcome. I’ve seen patients thrive post-treatment—returning to jobs, hobbies, families. My role is to maximize that potential with expert care and unwavering support.
Final Thoughts
Aneurysms and AVMs are daunting, but they’re not invincible. With over ten years of precision surgery and patient-centered care, I’m here to guide you through diagnosis, treatment, and recovery. If you’re facing symptoms or a diagnosis, don’t wait—reach out. Together, we’ll protect your brain and your future.
Dr. Shyam D is a distinguished board-certified neurosurgeon in India, with over a decade of expertise in intricate brain and spine surgeries. Known for his precision and compassionate care, he transforms lives through advanced vascular treatments.
